What can be done to reduce the risk of developing more skin cancer if they have already had basal or squamous cell skin cancer?
Surgical Excision in Fort Washington, PA
ABOUT SURGICAL EXCISION
One of the most recognized melanoma skin cancer solutions is surgical excision. During this procedure, Dr. Aradhna Saxena will surgically remove the melanoma or cancerous growth, along with the bordering tissue, which may appear to be normal. The excised tissue will be sent to a pathologist for further testing to determine whether or not the tissue border is cancer free. If the tissue proves to be cancerous, a subsequent procedure would be needed to remove the remaining cancer. At the Dermatology and Skin Cancer Institute, Dr. Saxena consults with Greater Philadelphia individuals on a regular basis to determine if surgical excision is the best treatment option for their melanoma skin cancer.
IDEAL CANDIDATES
You are likely a candidate for surgical excision if you have skin cancer on your arms, legs, or torso. This technique is thought to be simpler and faster than other surgical removal techniques, but it is not as cosmetically inconspicuous, meaning you are more likely to have an obvious scar. This technique is sometimes utilized to allow for continued observation of the skin cancer sample, so those in need of further diagnostic testing are also candidates for surgical excision.
SURGICAL TECHNIQUE
Since surgical excision is an invasive procedure, anesthesia will be given. For smaller, easier-to-reach melanomas, a local anesthetic will be administered. If a melanoma is larger and in a more difficult location, general anesthesia may be required. Prior to surgery, your treatment areas will be cleaned and prepared, and the anesthetic will be administered. Dr. Saxena will then remove the cancer using a scalpel and horizontal cuts around the growth and surrounding tissue. An electrode can be used to perform a feathering technique, which will smooth the edges around the wound. This helps to remove extra cells from the growth and minimizes the appearance of any scarring.
Small excisions can be stitched closed, while larger excisions may require a skin graft to close up the wound. A chemical will be applied to the treatment area to stop any bleeding, and an antibiotic will be prescribed to accelerate the healing process. In addition, a sterile bandage will be applied to the wound to protect it and keep it from getting infected.
WHAT TO EXPECT
The length of recovery and downtime after a surgical excision of skin cancer depends on the location and size of the particular excision, as well as whether skin grafts were required to complete the treatment. After your surgery, you may experience a burning sensation or general discomfort in the area where the skin cancer was removed. For the first few days following the surgery, we will advise you to take an over-the-counter medication, such as acetaminophen, to alleviate pain. You can also expect some scarring, which will appear red at first but will lighten over time. Many creams or gels can be applied to help lighten the scar. To protect the wound, a bandage should be placed on the treatment site when in the sun.
FREQUENTLY ASKED QUESTIONS
What is the difference between surgical excision and Mohs surgery?
Mohs surgery is a surgical excision; however, it is a more precise method that is typically used in areas that are more delicate or more visible, such as around the eyes, nose, and mouth, because it leaves more of the surrounding tissue intact than regular surgical excision. Regular surgical excision is a quicker surgery and may be a better option for larger or more aggressive skin cancer lesions.
How long will I take to heal?
Most patients take 1 – 3 weeks to heal from a surgical excision, but this differs for every patient and depends on the size of the excision. For patients who need a skin graft after their excision, it can take longer to heal. Dr. Saxena will talk with you about after care and recovery times for your unique case during your consultation and after your surgery.
Will I need another surgery?
Dr. Saxena’s goal with every excision is to remove all the cancerous tissue. However, once the removed tissue is tested at a lab, it may be determined that some cancerous tissue remains at the site on your body. In these cases, you will need to have a second surgery to ensure that all of the remaining cancer is removed.
Can my skin cancer come back?
The majority of patients who undergo excision surgery for basal cell or squamous cell carcinoma do not have a recurrence of skin cancer at the excision site. However, they can still develop skin cancer in other areas. If you’ve had skin cancer or have a family history of skin cancer, it is very important that you have yearly or twice-yearly skin cancer screenings at the Dermatology and Skin Cancer Institute of Greater Philadelphia.
SKILLED MELANOMA TREATMENT
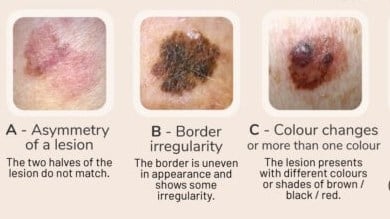
If you have a growth, lesion, or mole that appears abnormal, you should seek medical attention as soon as possible. It could be cancerous, and the sooner it is discovered, the better your chance for successful treatment before it spreads to surrounding skin and body parts. Make an appointment at the Dermatology and Skin Cancer Institute as soon as you can to meet with Dr. Saxena, who will examine the growth and discuss all your options, including whether surgical excision is appropriate.